Dr. Kumar’s Take:
This 2004 paper flips the traditional heart disease narrative on its head. Instead of blaming cholesterol as the cause of atherosclerosis, the authors suggest that inflammation comes first, and the body raises cholesterol levels as part of its effort to repair inflamed or damaged tissues.
Actionable Tip: Rather than focusing only on lowering cholesterol, it may be wiser to target root causes of inflammation — through diet, sleep, stress reduction, and addressing chronic infections or metabolic dysfunction.
Key Takeaways:
✔ Inflammation may trigger the rise in cholesterol — not the other way around.
✔ Lipoproteins might serve as protective, immune-modulating agents during inflammation.
✔ Atherosclerosis could be a consequence of chronic inflammatory signaling, not a primary lipid disorder.
Brief Summary:
This paper proposes that inflammation is the primary trigger for atherosclerosis — not high cholesterol. The authors suggest that lipoproteins like LDL, VLDL, and even Lp(a) are actually mobilized by the body in response to inflammation, acting like part of the immune system. These particles help neutralize damage and repair tissues. But when inflammation is chronic or uncontrolled, lipids accumulate excessively, and plaques begin to form in artery walls.
Study Design:
This was a conceptual and literature-based review, not a clinical trial. The authors analyzed data from immunology, lipid biology, and evolutionary biology to propose a new model for understanding cardiovascular disease. They examined how lipoproteins behave in the context of infection and injury, and suggested that their accumulation in arteries is part of a repair process — not the initiating factor in disease.
Results:
- LDL and other apolipoprotein B-containing lipoproteins may act like acute-phase reactants — rising in response to tissue injury or immune stress.
- The body uses lipoproteins to bind and neutralize inflammatory substances and repair tissues.
- Low HDL (and high LDL or VLDL) may signal ongoing inflammation rather than causing it.
- Treating inflammation may naturally improve lipid profiles and reduce cardiovascular risk.
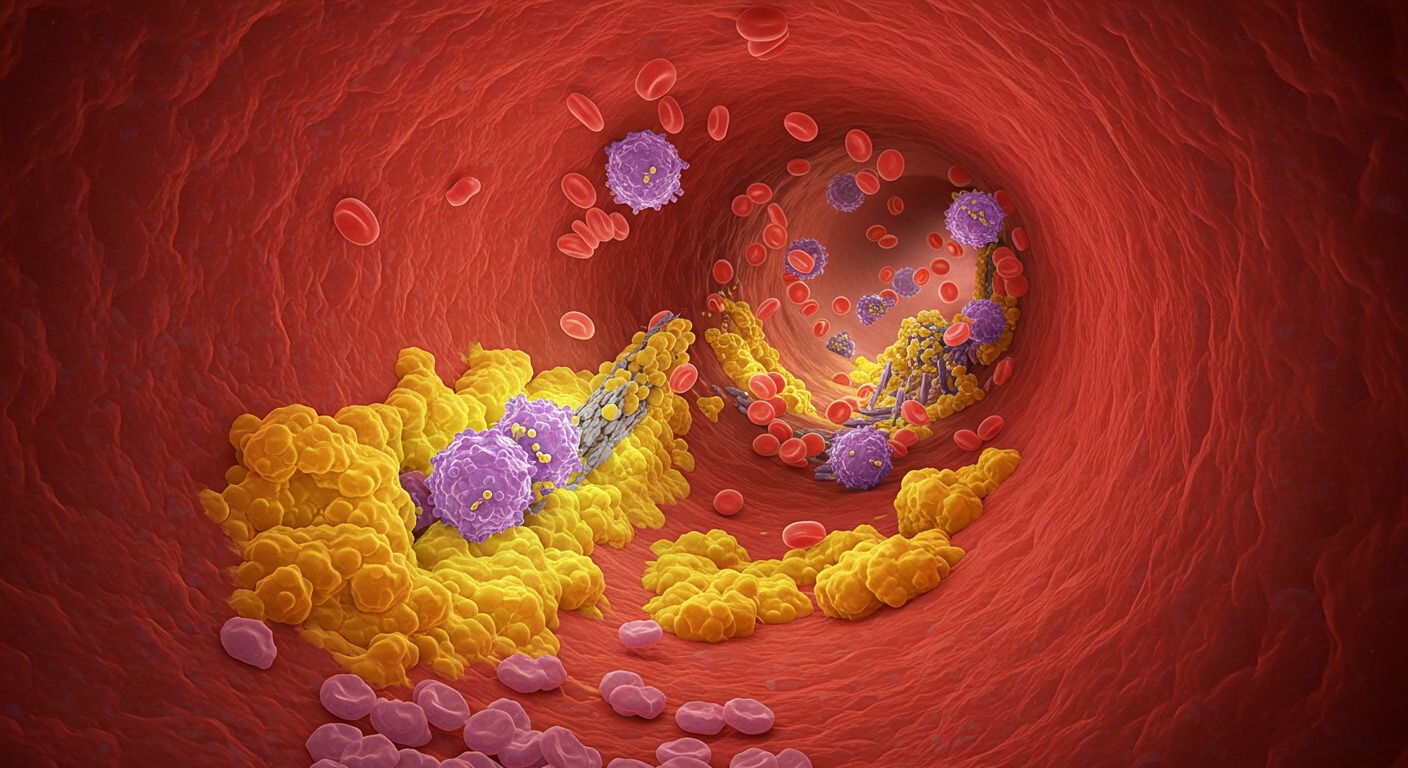
How Inflammation Triggers Cholesterol
According to this study, inflammation — from infections, metabolic dysfunction, toxins, or other sources — causes blood vessels to become damaged or dysfunctional. The body then ramps up lipoproteins like LDL to help repair that damage. LDL carries cholesterol and other molecules that play roles in patching tissues and neutralizing harmful substances.
Over time, if inflammation doesn’t resolve, these repair efforts go awry. Cholesterol particles can build up in the arterial wall, creating the plaques associated with atherosclerosis. But importantly, this buildup is secondary — the real problem starts with inflammation.
Related Studies and Research
Inflammation and Cardiovascular Disease – Discusses the broader role of inflammation as a root cause and driver of cardiovascular pathology.
Genome Evolution and Cardiovascular Risk – Examines how inherited genetic traits may contribute to modern cardiovascular risk through inflammatory pathways.
ApoB vs. LDL Cholesterol: Which is the Better Risk Marker? – Compares key lipid biomarkers in predicting heart disease risk, especially when inflammation is present.
PCSK9 Inhibitors and Cardiovascular Risk – Analyzes LDL-lowering therapies and their role in inflammation-independent cardiovascular protection.
Internal links to related studies coming soon.
Frequently Asked Questions
Does this mean cholesterol isn’t important?
Not exactly. Elevated LDL can still contribute to plaque buildup — but this paper argues that it’s more a sign of inflammation than a root cause. Lowering LDL may help, but addressing why it’s elevated matters more.
How can I reduce inflammation?
Anti-inflammatory habits include:
- Eating whole, unprocessed foods
- Avoiding excess sugar and seed oils
- Sleeping 7–8 hours a night
- Managing stress and staying active
- Treating chronic infections or gut issues
Is there a test to check my inflammation levels?
Yes. Talk to your doctor about:
- hs-CRP (high-sensitivity C-reactive protein)
- Fibrinogen
- IL-6
- Ferritin (can reflect inflammation)
Should I still take cholesterol-lowering meds?
That’s a personal decision based on risk factors. This study suggests focusing more broadly on inflammation and lifestyle — but medications may still be useful in certain situations. Always consult your doctor.
Conclusion
This paper argues that we’ve been looking at heart disease backwards. Instead of cholesterol causing inflammation and plaque, it may be that inflammation leads to cholesterol buildup, as the body tries to repair damage. If true, this has big implications for how we prevent and treat heart disease.
Treating the underlying inflammation — not just lowering cholesterol — could be the real key to protecting your heart.